Fistula
- Home
- Fistula
Fistula
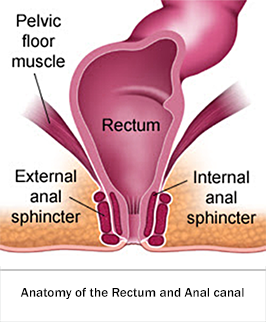
An anal fistula ( Bhagandar / Fistula in ano ) is a small channel that develops between the end of the bowel and the skin around the anus. It frequently is the result of a previous or current anal abscess. Fistula has a tract with two openings – Internal opening into the rectum or anal canal and External opening through the skin of the buttocks
Anal Fistula Treatment
Very few anal fistulas heal by themselves and the only effective cure for a persistent anal fistula is surgery.
Why get your fistula ( Bhagandar ) treated at Noble Surgicare Hospital ?
Till date, more than 1,000 patients have been successfully treated by Dr Vishal Pawar at Noble Surgicare Hospital. Extremely difficult cases of Complex fistulas and Recurrent fistulas ( those that have been unsuccessfully operated upon before ) have been efficiently managed at NSH. Dr Vishal Pawar is a renowned fistula doctor in India. Team of doctors and surgeons have successfully cured rare cases of fistula, like those extending from rectum to abdomen ( Recto-abdominal ), rectum to groin ( Recto-inguinal ), rectum to tailbone ( Recto-nidal ).
Giving an impetus to the existing armamentarium for treating fistulas, Laser surgery FiLaC ( Fistula-tract Laser Closure ), Distal Laser Proximal Ligation ( DLPL ) are the sphincter-saving procedures with negligible recurrence rate compared to all other techniques.
Noble Surgicare Hospital is a certified centre of excellence for fistula treatment in Navi Mumbai providing fistula care in Ulwe, Karanjade (Panvel), Dronagiri (Uran), Seawoods & Sanpada.
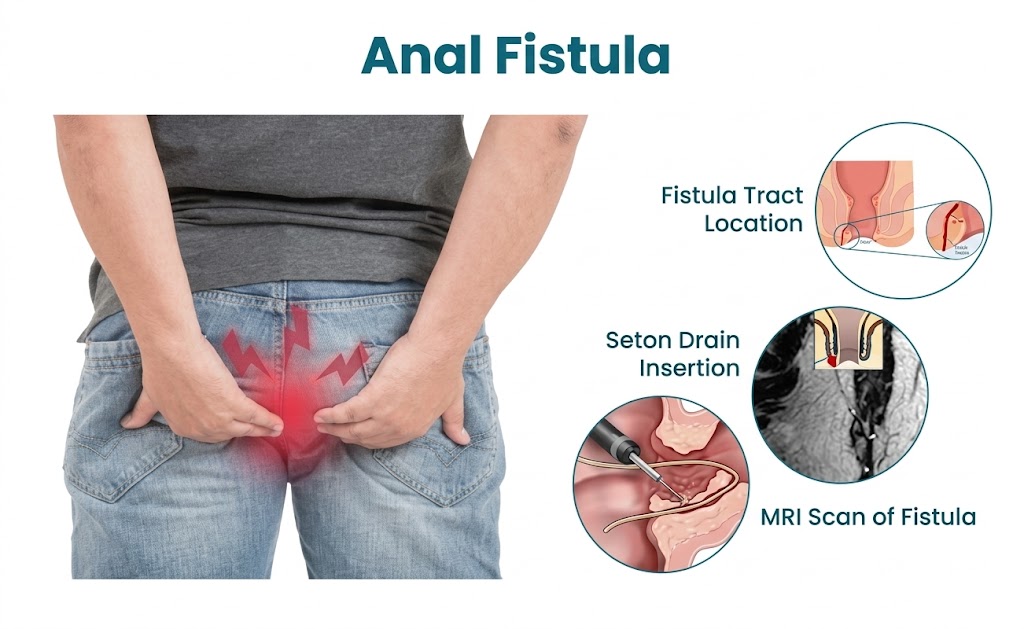
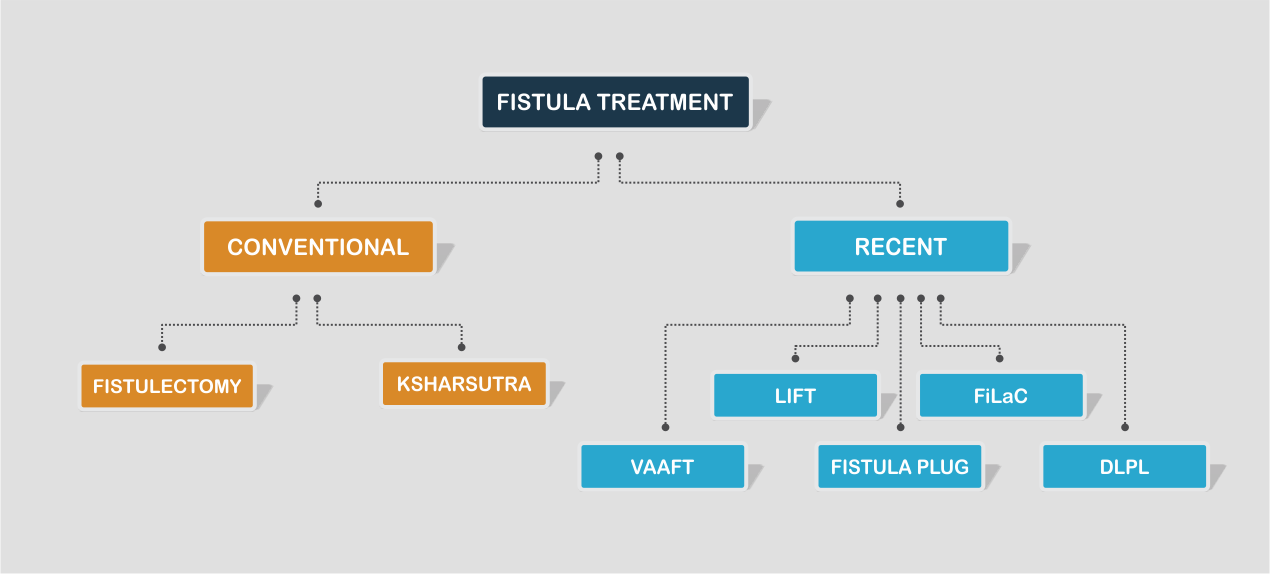
Fistula-in-Ano Treatment Methods
Learn More About Your Treatment
I. FISTULECTOMY
This is a surgical procedure in which the fistula tract is completely excised. Done under Spinal or General anaesthesia, the fistula tract is removed and the groove that is formed is left behind to heal. This procedure carries with it the risk of damage to the sphincter muscle resulting in fecal incontinence and is usually reserved as a treatment option for Complex fistula.
At Noble Surgicare Hospital, Laser is used as an adjunct to Fistulectomy to minimize the risk of damage to the sphincter muscle. Thus, with the added advantage of Laser the chances of post-operative incontinence are negligible.
II. KSHARSUTRA
This is an ancient Ayurvedic technique in which a special thread is used to treat the fistula. This thread is coated with Ayurvedic preparations and is inserted into the fistula tract.
The local irritation caused by the alkaline thread causes chemical cauterisation leading to inflammation within the tract. As a result the tract begins to debride. An important action of the Ksharsutra is that it allows continuous drainage of pus and debris from the tract. As all the infected material is drained, healing begins in a clean environment.
Advantages of Ksharsutra
- Non-invasive technique. Therefore no cuts and stitches.
- No damage to the sphincter muscle
- Fairly good success rate.
Potential drawbacks of Ksharsutra
- Multiple weekly sessions of treatment needed. So it’s a long treatment that is completed over a few months.
- The thread is a source of irritation. So there may be persistent local burning and pain.
- It is comparatively less effective in recurrent and complex fistulas.
III. VAAFT ( Video Assisted Anal Fistula Treatment )
The VAAFT technique is used for the surgical treatment of Complex fistulas. It is performed with the use of a fistuloscope. The procedure consists of 2 phases
- Diagnostic stage: In this phase your surgeon will identify the external opening of the tract through which the scope is introduced. Once this is done, the entire tract and any accessory tracts are delineated.
- Treatment stage: During this phase the inner side of the tract is fulgurated from the internal opening towards the external opening. This is followed by cleaning of the tract and closing the external opening.
Advantages
- No surgical wounds on the buttocks or perianal region.
- The internal opening is precisely located which is important in the treatment of any fistula.
- No damage to the sphincter muscle
Potential drawbacks
- The biggest argument against VAAFT is its high rate of recurrence (~30%)
IV. LIFT ( Ligation of Interspincteric Fistula Tract )
This procedure is usually performed for Complex or Deep fistulas. A seton is first placed in the fistula tract, forcing it to widen over time. A few weeks later, the surgeon removes the infected tissue and closes the internal fistula opening. The advantage of this procedure is that the fistula is accessed between the sphincter muscles thus avoiding cutting them. However, the success rate of LIFT is ~70% with an impaired healing in 20-30% cases.
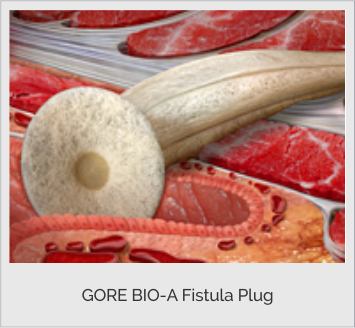
V. FISTULA PLUG
The fistula plug is a 100% synthetic bio-absorbable scaffold. This plug is placed in the fistula tract. Over time cells from the body migrate into the scaffold and new tissue is generated as the body gradually absorbs the plug material, leaving no permanent material in the body.
Advantages of Fistula Plug
- No cutting involved and no operation wound. Therefore it is associated with less pain and faster recovery.
- No damage to the sphincter muscle.
Potential Drawbacks
- Failures can occur due to dislodgement of plug from the fistula tract.
- The plug can get infected
- Failure of treatment can occur in 25-30% cases
VI. FiLaC ( Fistula-tract Laser Closure )
This procedure, done using the Lesotronics Laser. The aim of the procedure is to gently remove the fistula tract without damaging the sphincter muscle.
The procedure is done under Spinal or short General Anaesthesia and requires about 30-40 minutes. A radially emitting Laser Fibre is inserted from the outside. A defined amount of laser energy is then emitted circumferentially into the fistula tract. The laser energy causes controlled photothermal destruction of the fistula tract causing it to collapse to a high degree. This also helps supports and accelerates the healing process.
Advantages of FiLaC
- It has an excellent healing rate as compared to all other techniques.
- The anal sphincter is preserved so there is no risk of post-operative incontinence.
- It can be done in complicated fistulas like recto-inguinal, recto-gluteal fistulas.
- It is safe in high risk patients like those with hypertension, cardiac ( heart ) problems and in senior citizens.
Potential drawbacks of FiLaC
- There may be local burning for some time
- Post-operative subcutaneous abcess : It is usually managed with medications and dressing.
- In rare cases it may need incision and drainage under local anaesthesia.
VII. Distal Laser Proximal Ligation ( DLPL )
Fistula is a complex disease. Ultimately the aim of any fistula treatment is not just to get rid of the existing fistula but:
1. To save the sphincter muscle and thus prevent incontinence.
2. To prevent recurrence, considering the nature of the disease
Most of the techniques like VAAFT, LIFT, FiLaC achieve the primary purpose of closing the fistula and saving the sphincter. However, they all have their own rates of recurrence. Considering how bothersome a fistula is, even a small chance of recurrence can be a concern for the patient.
Dr Vishal Pawar, having specialised in Proctology ( a branch of surgery which deals with the rectum and gluteal region), has treated a large number of Fistula cases. In his experience of treating fistula patients over the past years, he tried to understand the nature of the disease and the cause of recurrences. After an in-depth study and applying all his knowledge and skills, he devised a technique he has labelled DLPL – Distal Laser Proximal Ligation.
In this procedure any abcess cavity along with the internal opening is first excised.This is followed by closure of the distal tract. The proximal part of the fistula tract is then sealed with the Leonardo Laser. With the radially emitting fibre of the laser, energy is applied circumferentially to the fistula tract. This ensures complete closure of the tract.
IN HIS SERIES OF 100 PATIENTS WITH COMPLEX HIGH FISTULAS TREATED WITH DLPL, THERE WAS NOT A SINGLE CASE OF RECURRENCE OR INCONTINENCE.
3D Endo-anal Imaging
Recently introduced 3D Endo-anal Pelvic Floor Imaging is an highly advanced, established technique for imaging the rectum and anal canal. It is rapid, simple and well-tolerated. It also provides valuable information about the anatomy of the anal sphincters.
Role of 3D Endo-anal Imagining in Fistula
Many patients suffering from Fistula are not diagnosed properly because of the complex anatomy and limited diagnostic options. Although MRI Fistulogram is a commonly used technique for Fistula imaging, many patients are claustrophobic or just fear getting inside the MRI machine. Besides, Fistula is a dynamic disease wherein new tracts and abscesses may form from time to time. Thus an old MRI may not give an accurate picture of the current disease. 3D Endo-anal Pelvic Floor Imaging is a patient-friendly procedure that can be done at any given time. The most important aspect of this technique is that it can be used intra-operatively, which means that the surgeon can use it while performing the surgery. Post-operatively, it is used to confirm the accuracy of the fistula repair.
India’s latest 3D Endoanal Imaging for Fistula/Abscess
3D Endoanal Imaging is an important tool to study the various characteristics of Fistula. Fistulae are visualised as hypoechoic tracts. Specific features like the site of internal opening, level of the radial tract, the relation of tracts to anal sphincters and site of fluid collections/pararectal cavities can be obtained. It provides a detailed multiplanar reconstruction of the anal canal. 3D Imaging is particularly helpful in high fistulae with anal sphincter involvement, especially if there are additional extensions and associated pararectal collections. It gives useful information about the sphincter defects which is important in planning surgery in order to minimise damage to anal sphincter complex.
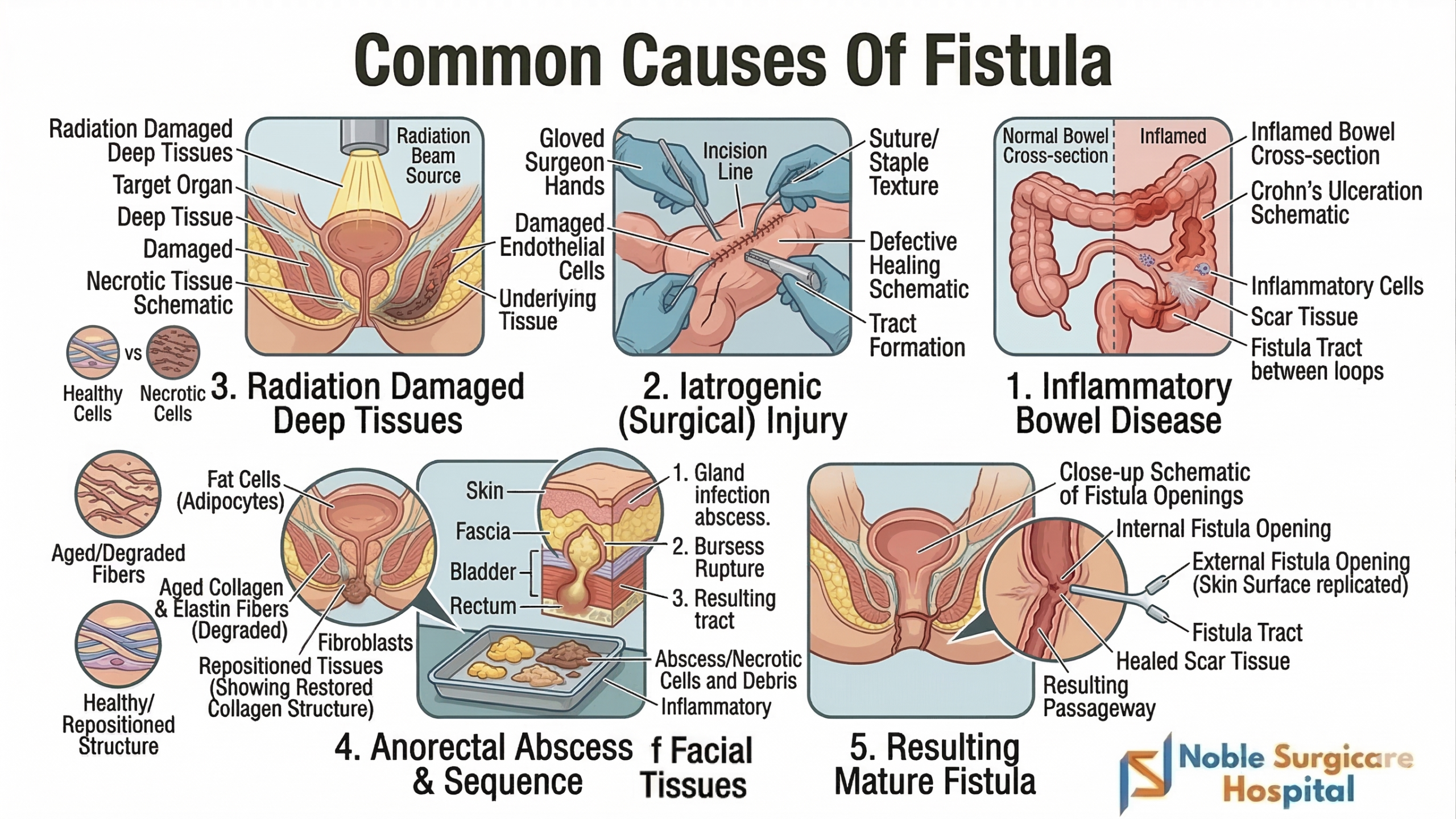
Causes Of Fistula
A fistula is an abnormal connection forming between two body organs or vessels. Most commonly, they develop due to untreated infections that create severe inflammation and tissue damage.
Surgical complications are another frequent cause of fistulas. Accidental injuries during complex operations or poor wound healing can inadvertently link structures, requiring careful medical evaluation and corrective treatment.
Chronic medical conditions significantly increase your risk. Inflammatory bowel diseases, specifically Crohn’s disease, frequently trigger fistulas by causing persistent internal swelling, deep ulcers, and continuous intestinal tract irritation.
Key Causes of Fistula:
-
Severe or untreated local infections (such as an abscess).
-
Complications or accidental injuries from recent surgical procedures.
-
Inflammatory Bowel Disease (IBD), particularly Crohn’s disease.
-
Tissue damage resulting from targeted radiation therapy.
-
Physical trauma or injury to the affected body area.
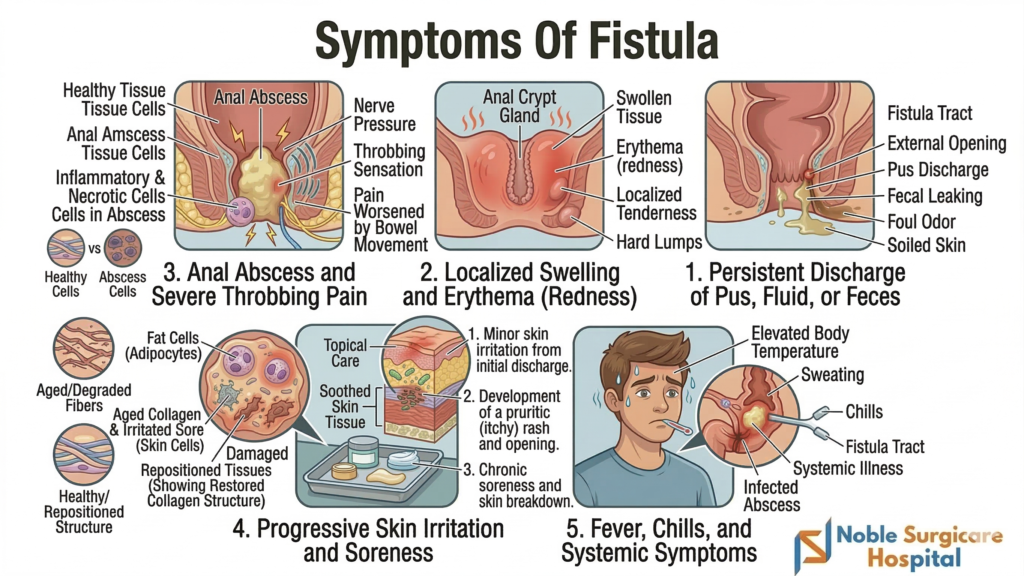
Symptoms of fistula
Individuals with a fistula often experience constant, throbbing pain in the affected area. This severe discomfort typically worsens significantly when sitting down or during a regular bowel movement.
Another prominent symptom is persistent drainage of blood, pus, or infected fluid from an external opening. This continuous leakage causes severe skin irritation and localized swelling around it.
If the internal tract becomes infected or blocked, patients may develop systemic signs of illness. Recurring fevers, sudden chills, and a general feeling of extreme fatigue frequently occur.
Key Symptoms of a Fistula:
-
Constant, throbbing pain that intensifies with movement or sitting.
-
Visible discharge of pus, blood, or foul-smelling fluid.
-
Skin irritation, redness, and tenderness around the external opening.
-
Recurrent abscesses or palpable hard lumps near the affected region.
-
Systemic signs of an active infection, including fever and chills.
Would you like me to draft the content for the “Diagnosis of Fistula” image next?
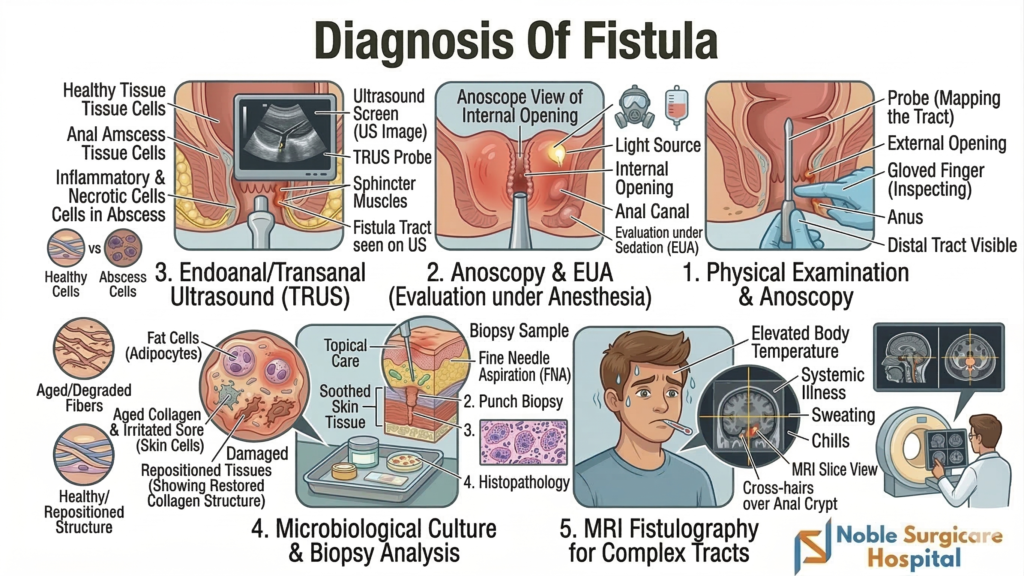
Diagnosis Of Fistula
A doctor begins diagnosing a fistula with a thorough physical examination of the affected area. They carefully check for visible external openings, signs of infection, and fluid drainage.
To determine the depth and direction of the abnormal tract, specialized medical instruments are utilized. A surgical probe helps map the pathway connecting the internal and external tissues.
For complex cases, advanced imaging techniques become absolutely essential for accurate evaluation. Doctors frequently order an MRI or endoscopic ultrasound to visualize deeper muscle layers and hidden complications.
Key Methods for Diagnosing a Fistula:
-
A comprehensive physical and visual medical examination.
-
Utilizing a medical probe to gently trace the tract’s path.
-
Performing an anoscopy to evaluate the internal canal tissues.
-
Using an endoanal ultrasound to assess surrounding muscle layers.
-
Ordering MRI scans for detailed imaging of complex fistula networks.
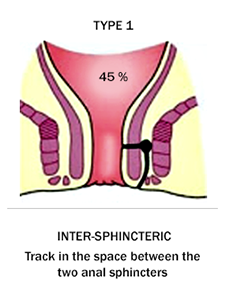
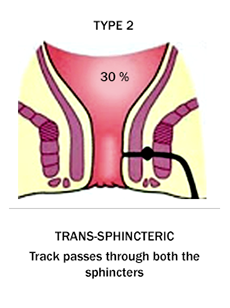
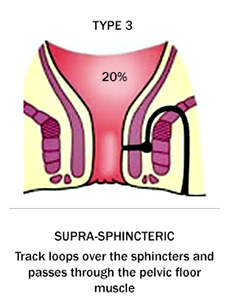
Types of Fistula
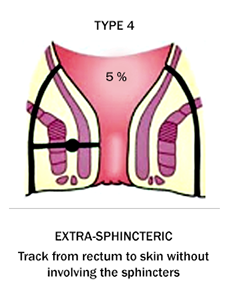
Frequently asked questions
Only a person who has suffered from fistula-in-ano knows what an irksome condition it is to have! In our long-standing experience of treating fistula cases, we have realised that a successful outcome of the treatment depends as much on the patient’s cooperation and self-care, as on the surgeon’s skill. Hence, we have answered a few queries which patients generally face during their fight against fistula.
What do I feel during the procedure?
It’s like taking a small nap! All you will feel is a small needle prick during your preparation for the procedure. The entire surgery takes about 30 minutes. Occasionally, only the lower half of your body is anaesthetised and you will be alert and probably having a chat with your doctor!
During laser surgery, is the laser probe inserted within the fistula tract to burn it? How does this help?
Yes, the laser probe is inserted within the fistula tract and the laser energy is applied circumferentially to coagulate ( burn ) it. The tract heals by a process called ‘secondary intention’.
What happens after the operation?
You will normally be able to start drinking water shortly after the procedure and can start eating as soon as you are hungry. You will be able to get out of bed a few hours after surgery.
You are likely to have some pain after the procedure that is easily controlled with painkillers.
When can I go home?
If your operation is planned as a day care procedure you can go home as soon as the effect of the anaesthetic has worn off, you have passed urine and you are comfortable, eating and drinking. Since a general anaesthetic is used, it is advisable that a responsible adult take you home and stay with you for 24 hours.
At times you may be given a discharge after 24 hours in which case you may need to stay in the hospital for a night.
Before you are discharged you will be advised about post-operative care, painkillers and laxatives.
Do I need to follow any specific diet before/after fistula surgery?
You do not need a specific diet. Just make sure you eat a healthy, fiber-rich diet before and after surgery.
What can I do to promote successful healing?
Get plenty of rest, take a Sitz bath about 3 times a day ( especially after a bowel movement ), maintain self-hygiene and consume a fibre rich diet.
In how many days can I start travelling after a fistula surgery?
You may start travelling after a week.
Do I need to use a special ( doughnut ) pillow while sitting?
You do not need any special pillow after surgery.
How long does it take for a Fistula to heal?
It may take 6-8 weeks for anal fistula to completely heal. Take complete rest for the first 24 hours after surgery. You can gradually resume your daily chores and most people are back to their normal activities in 5-7 days.
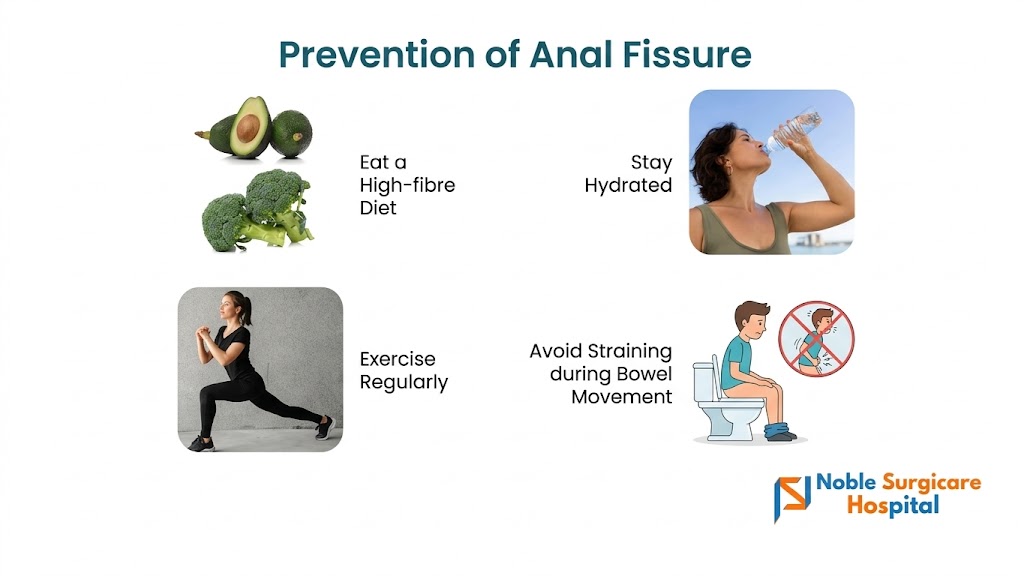
Treatment of Fistula
The primary treatment for a fistula is surgery, as they rarely heal on their own. A fistulotomy is the most common procedure, where the surgeon opens the entire length of the tunnel to allow it to heal from the inside out.
For complex fistulas passing through sphincter muscles, a seton placement may be used. A surgical thread is placed in the tract for several weeks to help drain infection and slowly heal the area while protecting muscle function and preventing incontinence.
Advanced options include ligation of the intersphincteric fistula tract (LIFT) or using medical glue and plugs. These minimally invasive techniques aim to close the internal opening without cutting the sphincter muscles, ensuring a safer recovery and preserving bowel control.

More Information
91+7977273728
